It’s a situation no one wants to be in. You are experiencing sharp, debilitating pain. This pain is not like your standard muscle soreness. This is nerve pain. You’re getting electric shocks, pins and needles, or burning sensations along your back or into your arms and legs. It’s gotten to the point where you are beginning to lose function in your daily life. You can barely make it through your workday. Let alone being able to go on that hike. You aren’t able to play with your kids or grandkids. You go and get yourself checked out by your doctor. After a whole battery of testing, it is determined that you have nerve impingement, disc herniation/degeneration or spinal stenosis.
Now what? At this point, most doctors are going to give you treatment options like; medicate to mask the pain, try physical therapy, get injections, or have spinal surgery to decompress your nerves. With today’s increasingly sedentary lifestyles, as well as the baby boomer generation advancing in age, rates of chronic back pain have continued to rise. From 2000-2007 the total number of adults in the US suffering from chronic back pain has increased by 64% (approx. 7.8 million to 12.8 million), with the average age of patients rising from 48.5 to 52.2. (Baber et al 2016). As a result, the number of surgeries has also increased over the same time period – 170% for spinal fusions (Rajaee et al 2012) and 11% of laminectomies (Parker et al 2015). What follows is some information to help answer some questions about what your options are when it comes to decompressive surgery, as well as a possible alternative to effectively treat your condition.
Conventional Pre-Surgery Treatments

Most often, there are a series of treatments that are recommended before surgery will be authorized. Typically, the first step is pharmaceutical. Prescription muscle relaxers, painkillers, and anti-inflammatory medications are tried. The next step is physical therapy. Exercise is essential for optimal health; however, exercise often exacerbates the pain if you have nerve compression. The last step before surgery typically is steroid injections. While they may provide temporary relief for inflammation, they rarely offer lasting relief for nerve compression. In the conventional medical treatment model, all that remains is spinal surgery.

Spinal surgery often consists of two procedures performed at the same time: a procedure to remove the tissues causing the nerve impingement, followed by spinal fusion. The most common type of decompressive surgeries are laminotomies and laminectomies. These procedures sound very similar, as they both involve the lamina of your spine. Each individual vertebrae in your spine have a lamina on either side of the posterior aspect which creates a bony arch that encases your spinal cord. A laminectomy involves complete removal of this bony arch as the lamina is totally removed, whereas a laminotomy will only remove a portion of bone that is causing the nerve impingement. The type of surgery you receive will be dependent on the extent of nerve compression and whether other procedures will need to be completed. To perform both a laminectomy and a laminotomy an incision is made at the vertebral level where the nerve compression is occurring. The tissue is opened, cutting through skin and dissecting muscle to expose the bone of the spine. In a laminectomy, the spinous process and lamina are completely removed from the vertebra in order to relieve the pressure caused by these structures on the nerve roots or spinal cord. These bony structures can be seen below in Figure 1. The spinous process is a bony landmark, they are the “bumps” you feel on your back under the skin. They serve as muscle attachment sites, while the lamina shown in red form the arch that covers your spinal cord. A laminotomy will keep some of these bony structures intact, but will still require removal of some of the lamina itself by cutting away the bone to decompress the nerve.
If these surgeries alone are not enough to completely decompress the nerve, the surgeon may elect to perform additional procedures before closing the initial entry incision. Depending on where the nerve compression is occurring this may call for a discectomy to remove part or all of a bulging/herniated disc. Finally, a foraminotomy may be performed to remove bone spurs or open- up the canals (foramen) where the nerve root exits the spine.
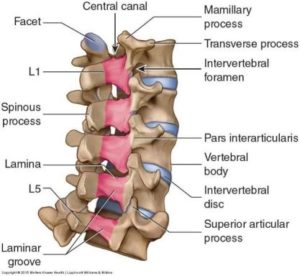
Figure 1. Bony anatomy of the Lumbar Spine featuring the lamina of each vertebra in red and the bony landmark of the Spinous Process.
With a laminectomy, removing these significant portions of bone creates the potential for instability in that region of your spine. In addition, some of the intrinsic muscles that are the primary stabilizers of the spine attach directly onto portions of the vertebra that are removed. Also, the surgeon has to cut through the paraspinal muscles to access the disc and lamina. These muscles are responsible for helping your back straighten out, rotate, and keep you upright. As a result, a laminectomy is often combined with a spinal fusion at that level, which requires the surgeon to drill screws into the vertebra above and below the affected level and connect them with steel rods.
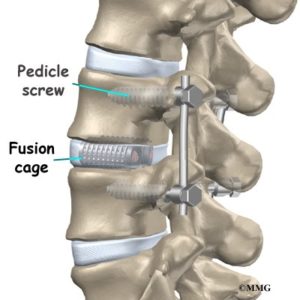
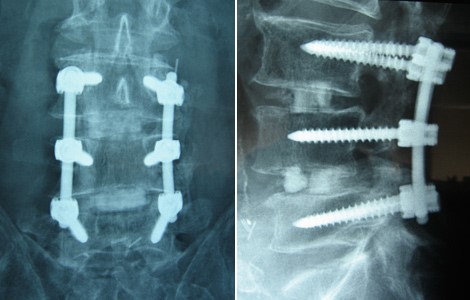
Figure 2.a Spinal fusion rods and screws. b. AP X-ray of lumbar fusion. c. Lateral X-ray of lumbar fusion
This hardware is required to maintain stability. This in turn creates a block of bones that can severely restrict normal ranges of motion. Meaning that even if the surgery is successful in reducing nerve compression, it comes at the cost of a permanent loss of normal movement. The result of this restriction can accelerate degeneration of the discs and joints above and below the fusion site resulting in pain, inflammation, and potentially additional surgeries. (Ma et al 2019).
Due to the invasive nature of the procedure and risks associated with anesthesia, surgery is not an option for some patients. This is often the case due to a patient’s age, immune competency level, etc. If surgery is not an option, commonly patients are told the only treatment available to them are pharmaceuticals to try to manage their pain.
Effectiveness
According to studies, somewhere between 10% and 74% (Nguyen et al 2011) of back surgeries fail. According to Dr. Steven Atlas, an associate professor of medicine at Harvard Medical School, “Your pain is typically decreased by 50 percent,” Dr. Atlas says, “but there are very few people who really have no pain after spinal fusion.” The relief may last only a few years before the condition worsens again.”
In addition, surgery is essentially an all or nothing event. The surgeon can’t go in, shave off a bit of bone, sew you up, and “see how you do”. The only reason that would even be considered an option, is if your condition is complicated enough to warrant multiple surgeries to correct the issue. Finally, a 2017 article from the journal World Neurosurgery found that one-fifth of patients 65 and over who received a spinal surgery had to be readmitted to the hospital due to complications (Aodgwa et al 2017).
Time and Cost of Decompressive Surgery

Many elective spinal surgeries are outpatient procedures, completed within a few hours. More serious cases could require some hospitalization. In addition, most surgeons will recommend that the patient do some sort of conditioning program before the surgery. This could include a few weeks of physical rehabilitation that occurs before the surgery. Then there is time lost from the surgery itself. Although it can be an outpatient procedure, most patients will not be able to return to work full time for days to weeks afterward. Finally, we come to the additional time and expense of doing rehabilitative physical therapy to rebuild strength and stability. For more information regarding the cost of surgical and non-surgical decompression, please reference our article Understanding Treatment Costs.
Is there another way to accomplish decompression?
Prompted by the poor success rate and high incidence of complications for spine surgery, non-surgical spinal decompression was invented. In 1991 a medical researcher, Dr Allan Dyer MD, PhD, created a therapy device to mechanically reduce nerve compression. Combining his medical understanding with basic physics principles, Dr Dyer reasoned that applying a sufficient axial load to the spine would create a vacuum in the disc that could reduce the protrusion of a herniated disc. It helped Dr Dyer get relief from his back pain and was quickly embraced by the conservative health care community.
Comprehensive Conservative Treatment
At Olympic Spine and Sports Therapy, all of our treatments are drug-free, non-surgical, safe, and pain-free. We use a unique and comprehensive treatment approach that provides lasting relief so you can regain your quality of life.
Treatment for spine-related conditions often includes:
- Non-Surgical Spinal Decompression, to reduce nerve pressure and repair damaged discs.
- Chiropractic adjustments and Joint mobilization, to restore proper motion.
- High Dose Laser, to reduce pain, and accelerate nerve repair.
- Skilled manual therapy, to restore muscle balance.
- Integrated Functional rehabilitation, to restore control, strength and endurance.
To learn more about our comprehensive treatments you can reference the article: Solutions for Sciatica and Chronic Back and Neck Pain, or view the video: Solutions for Chronic Spine Pain
Non-Surgical Spinal Decompression

Although each of the therapies we use contributes to the healing process, non-surgical decompression is the chief treatment for nerve compression and disc conditions. As explained previously, spinal decompression machines gently stretch the spine, creating a vacuum inside the discs and joints. The negative pressure can reduce disc bulges, draw nutrients and water into the disc, reduce swelling and inflammation, and improve joint motion.
Below are MRI images of a patient with a disc herniation at L5-S1. The before picture clearly demonstrates the disc bulging into the spinal canal. The after picture was taken following a course of treatment including spinal decompression and shows a reduction of the herniation.
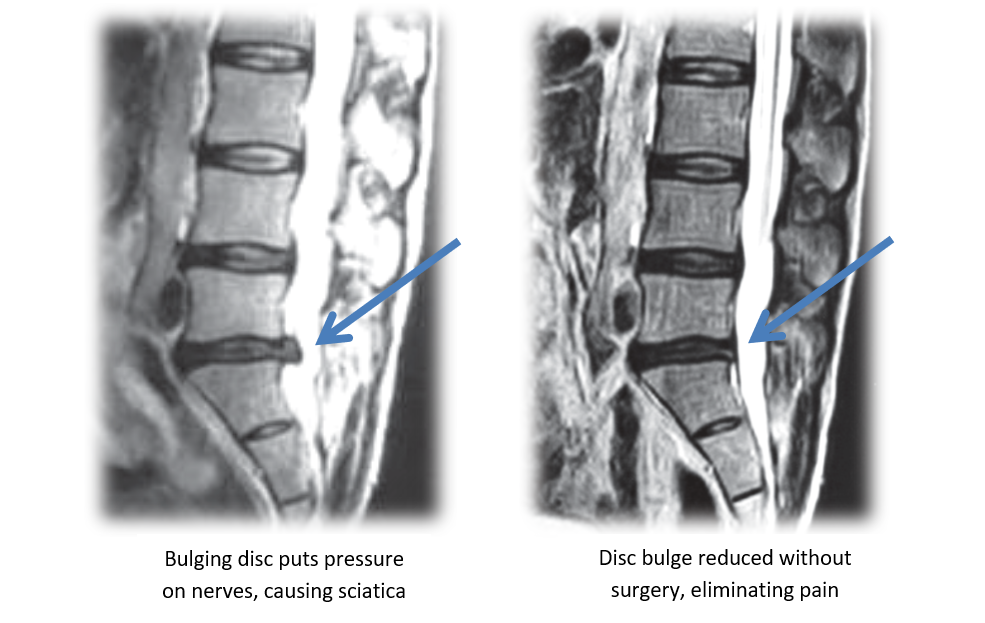
Non-surgical decompression machines are not the same as inversion or traction units. With inversion, traction force is generated by hanging from your ankles or knees, the only control over the force is the angle you hang at. The force is static unless you move. With a spinal decompression machine, the force is controlled and directed. The rate of application of pressure, the maximum and minimum levels of force and length of pressure application are all programmed into the machine. The cycling of the pressure, like a sign wave, /\/\/\/\ produces a pumping action that improves circulation. This is particularly important where disc conditions are concerned since discs do not have a direct blood supply. In addition to being effective, spinal decompression is safe and pain-free. Our decompression machines are FDA cleared and can be turned off by the patient if they have any discomfort. Most patient’s decompression is so comfortable and relaxing, they can take a nap during their treatment.
Who Will Non-Surgical Decompression Work for?
At Olympic Spine and Sports Therapy, we have been able to help thousands of patients find relief from symptoms due to disc conditions and nerve compression. We have accomplished this without the use of drugs, injections or surgery. To be clear, we believe there is a time and place for surgery. If comprehensive conservative treatment is not successful, surgery may be the only option. To determine if a patient is a candidate for spinal decompression, we take a detailed history, perform a comprehensive orthopedic and neurological examination and order X-Ray, MRI, CT, and electrodiagnostic tests as indicated. If from this evaluation we determine a patient is a candidate for treatment, we provide recommendations outlining the specific therapies, their frequency and duration, and re-evaluation improvement expectations. At Olympic Spine and Sports Therapy, we believe the best treatment for a patient, is the treatment that is the safest, most effective, and least expensive. We provide consultations free of charge to determine if a patient is a good candidate for care. To schedule a consultation you can call us at 425-967-6426 or email us at help@olympicspine.com. We would like nothing more than to help you find relief and regain your ability to live your life.
Adogwa O, Elsamadicy AA, Han J, et al. Drivers of 30-Day Readmission in Elderly Patients (>65 Years Old) After Spine Surgery: An Analysis of 500 Consecutive Spine Surgery Patients. World Neurosurgery. 2017 Jan;97:518-522. DOI: 10.1016/j.wneu.2016.07.032.
Baber Z, Erdek MA. Failed back surgery syndrome: current perspectives. J Pain Res. 2016;9:979‐987. Published 2016 Nov 7. doi:10.2147/JPR.S92776
Ma Z, Huang S, Sun J, Li F, Sun J, Pi G. Risk factors for upper adjacent segment degeneration after multi-level posterior lumbar spinal fusion surgery. J Orthop Surg Res. 2019;14(1):89. Published 2019 Mar 28. doi:10.1186/s13018-019-1126-9
Nguyen TH, Randolph DC, Talmage J, Succop P, Travis R. Long-term outcomes of lumbar fusion among workers’ compensation subjects: a historical cohort study. Spine (Phila Pa 1976). 2011;36(4):320‐331. doi:10.1097/BRS.0b013e3181ccc220
Parker SL, Mendenhall SK, Godil SS, Sivasubramanian P, Cahill K, Ziewacz J, McGirt MJ. Incidence of low back pain after lumbar discectomy for herniated disc and its effect on patient-reported outcomes. Clin Orthop Relat Res. 2015;473(6):1988–1999.
Rajaee SS, Bae HW, Kanim LE, Delamarter RB. Spinal fusion in the United States: analysis of trends from 1998 to 2008. Spine. 2012;37(1):67–76.